Can you really make a good living for yourself as a yoga therapist? How much do yoga therapists make an hour, and how do you know what to charge your clients? Many people are interested in the intersection of physical therapy and yoga techniques, but few know much about the yoga industry and whether it’s possible to earn a living doing what they love.
That’s about to change! This comprehensive guide covering everything from industry norms to the average yoga therapy salary will serve as your guide to earning as a yoga therapist. It’s important to understand that there are many factors that affect how much you will earn, so get started with the data we’ve presented and the expert insights provided by our Founder, Director, and Lead Teacher, Brandt Passalacqua.
Yoga Therapist Salary Ranges

A yoga therapist’s annual salary can range from $59,000 to $100,500, according to ZipRecruiter. The national average yoga therapist salary is $70,000, with most salaries ranging from $63,500 to $70,000.
| Percent of Yoga Therapist Jobs | Salary Range |
| 17% | $59,000–$62,499 |
| 27% | $62,500–$66,499 |
| 32% | $66,500–$69,999 |
| 18% | $70,000–$73,999 |
| 4% | $96,500–$100,500 |
This broad range suggests that there are plenty of opportunities for advancement within the profession. Yoga therapists may run their own private practice or work at a clinic which will affect their salary along with other factors in the next section.
Factors That Affect Yoga Therapist Salaries
With such a wide range of yoga therapist salary amounts, there are several elements that factor into how much yoga therapists make.
- Location: Location perhaps plays the biggest role in the variation of salaries. The location of one’s business and cost of living will affect a yoga therapist’s salary. Yoga therapy rates in urban areas are typically higher than rural locations.
- Experience: The years of experience a yoga therapist has will also affect how much they charge and, in turn, their salary. Just as any other career, in general, people with more years of experience make more money.
- Skill Level: Skill level also plays a part in a yoga therapist’s salary. Certifications and specialized training and development can increase a yoga therapist’s salary. There are even master’s degrees in yoga therapy, though most yoga therapists don’t need a master’s to get a job or advance their career.
- Private Practice or Public Clinic: Yoga therapists that own a private practice may expect to make more money than those who work for a clinic, as they can set their own hourly or session rates. Take notice that private practice salaries are still influenced by location, experience, and skill level.
Listen to an overview of some of these factors in this video segment with our Founder, Director, and Lead Teacher, Brandt Passalacqua. He explains to one of our students how to determine your hourly rates and the variation in yoga therapist salary for both a private yoga therapy practice and a yoga therapy clinic.
In this segment, Brandt discusses hourly rates and a yoga therapist salary for both a private Yoga Therapy practice and a Yoga Therapy clinic.
Transcription
Brandt Passalaqua: So, what was your question? You were asking about rates and yoga therapist salaries?
Student: Yes, how do you guys decide to set your yoga therapy rate.
Brandt: You have two options, but for private rates, I would look at what acupuncturists charge, massage therapists charge, and psychotherapists charge, because, you know, like in New York City, people get $120, or $150, or $200 an hour. You know what I mean?
Student: Yes.
Brandt: Two hours away, where I live, people get $90. If I went an hour and a half from my house to Vermont, people are probably more likely to get $75, as you are getting further away from the cities.
Student: Okay.
Brandt: But, I would look at it that way. And the other option is something I’m working on now, is doing it in a different style – like a clinic style – where it depends on how much money you need, but where you set up a Yoga Therapy clinic or a couple of clinic days, and you do shorter appointments and charge less. So, I’m going to be giving everyone protocols for that because I’m working on that right now, sort of ironing that out. It’s also a good way to get into the community. So, a lot of other alternative medical professionals work that way, where you have for example two days a week of regular office hours and you charge your full rate, let’s say that’s $90 an hour, and then you have a Yoga Therapy clinic day where people can come for half an hour for $30 for example, so you’re working with both sets of populations. So, that would be another way to think about it.
How Much Do Yoga Therapists Make an Hour?
On average, yoga therapists make $33.65 an hour in the U.S., according to ZipRecruiter. But this is based on annual salary and assumes the number of hours worked. In reality, many yoga therapists will command a higher hourly rate than $33.65 an hour. Depending on your experience, location, and other factors, you may be more likely to charge clients upwards of $100 an hour.
Location, experience, skill level, and working in a private practice versus a public clinic will all affect how much yoga therapists make an hour, however. Keep this information in mind and keep reading to learn more about these different factors so you can make an informed decision about what to charge.
How Much Does a Yoga Therapist Make in My State?
When determining how much to charge for yoga therapy, consider the average yoga therapist salary and hourly wage in your state. But keep in mind that how much a yoga therapist makes will also vary from city to city within each state, with bigger cities generally charging higher prices and having higher cost of living than smaller cities. Check out data from ZipRecruiter below to give you an idea.
| State | Salary (Annual) | Hourly Wage |
| New York | $79,854 | $38.39 |
| California | $78,793 | $37.88 |
| Vermont | $72,011 | $34.62 |
| Maine | $71,542 | $34.40 |
| Massachusetts | $70,975 | $34.12 |
| Nevada | $70,839 | $34.06 |
| New Jersey | $70,071 | $33.69 |
| Wisconsin | $69,922 | $33.62 |
| Washington | $69,752 | $33.54 |
| Oregon | $69,085 | $33.21 |
| Hawaii | $68,251 | $32.81 |
| Idaho | $68,235 | $32.81 |
| Wyoming | $68,111 | $32.75 |
| Minnesota | $67,750 | $32.57 |
| Indiana | $67,417 | $32.41 |
| Arizona | $67,396 | $32.40 |
| Alaska | $67,000 | $32.21 |
| New Hampshire | $66,843 | $32.14 |
| Pennsylvania | $66,799 | $32.11 |
| Georgia | $66,252 | $31.85 |
| Iowa | $65,332 | $31.41 |
| Rhode Island | $65,254 | $31.37 |
| South Dakota | $65,161 | $31.33 |
| North Dakota | $65,112 | $31.30 |
| Connecticut | $64,752 | $31.13 |
| Montana | $64,658 | $31.09 |
| New Mexico | $63,315 | $30.44 |
| Illinois | $63,023 | $30.30 |
| Ohio | $63,016 | $30.30 |
| Virginia | $61,960 | $29.79 |
| Maryland | $61,877 | $29.75 |
| Tennessee | $61,678 | $29.65 |
| Utah | $61,644 | $29.64 |
| Delaware | $60,970 | $29.31 |
| Colorado | $60,709 | $29.19 |
| Mississippi | $60,207 | $28.95 |
| Oklahoma | $58,866 | $28.30 |
| South Carolina | $58,600 | $28.17 |
| Michigan | $58,084 | $27.93 |
| Kansas | $57,880 | $27.83 |
| Texas | $57,796 | $27.79 |
| Missouri | $57,737 | $27.76 |
| West Virginia | $57,557 | $27.67 |
| Alabama | $56,955 | $27.38 |
| Florida | $56,894 | $27.35 |
| Louisiana | $56,489 | $27.16 |
| Nebraska | $56,144 | $26.99 |
| Kentucky | $53,864 | $25.90 |
| North Carolina | $53,504 | $25.72 |
| Arkansas | $52,987 | $25.47 |
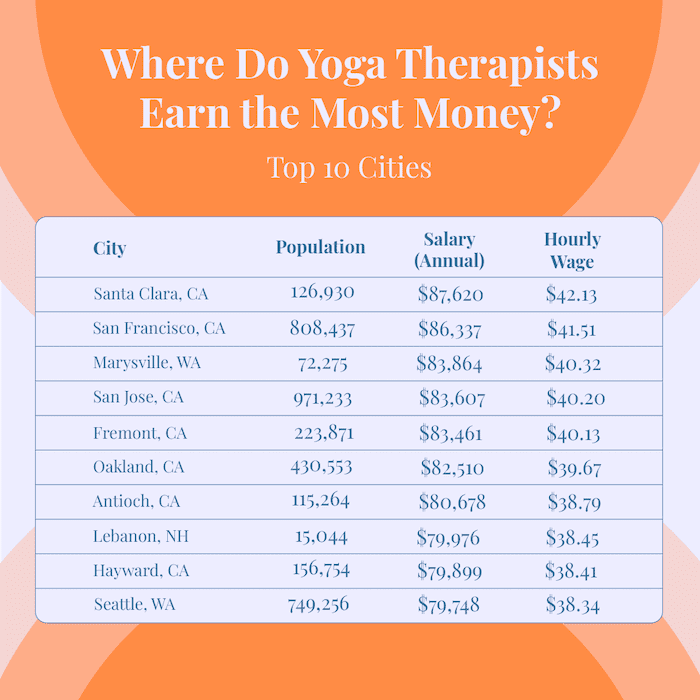
Where Do Yoga Therapists Earn the Most Money? Top 10 Cities
If you’re looking for the cities where you could have higher earning potential, check out the top 10 cities for the highest yoga therapist salaries according to ZipRecruiter below. While you can generally charge more for yoga therapy in bigger cities like San Jose, San Francisco, or Seattle, there are a few smaller cities like Lebanon, New Hampshire or Marysville, Washington on this list to consider if you prefer small town life. Just keep in mind that a smaller population may mean a smaller demand and clientele as well.
Yoga Instructor vs. Yoga Teacher vs. Yoga Therapist Salary
The average person may be surprised that there’s a difference between yoga therapists and yoga teachers. Yoga teachers and instructors teach yoga classes, which can be one-on-one or in a group. Yoga therapists teach clients how to use yoga techniques to provide relief for the specific medical conditions they face.
Yoga therapists typically focus on specific health conditions and can provide more specialized medical advice. Yoga teachers may be more junior, focusing on teaching students about the various yoga systems (e.g. Ashtanga vs. power yoga) because they lack specific credentials needed to carry out more intensive therapy sessions.
A yoga therapist’s salary will thus depend more heavily on their experience, practical knowledge, and demonstrable ability to treat patients. A yoga teacher who is more personable, skilled at educating others, and familiar with the industry basics may make a nice living for themselves but will seldom draw in the highest wages without additional training.
Yoga therapists play an important role in many people’s health. They use mind and body practices, such as breathing techniques and stretches, to promote deep relaxation and healing. The needs of the client determine the yoga therapy practices that are used.
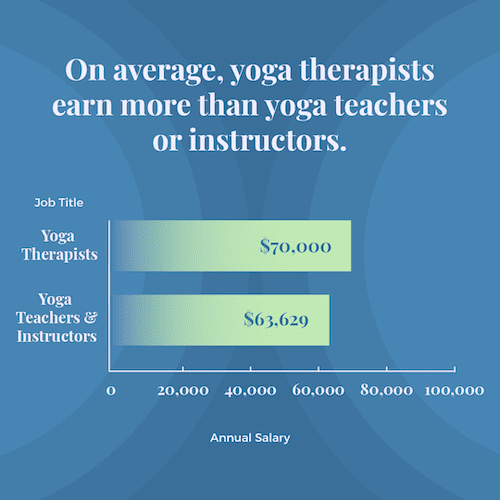
Due to these differences, there are some differences in yoga instructor or yoga teacher and yoga therapist salaries. The average yoga therapist salary in the U.S. is $70,000 annually ($33.65 per hour), compared to $63,629 annually ($30.59 per hour) for yoga teachers and yoga instructors, according to ZipRecruiter.
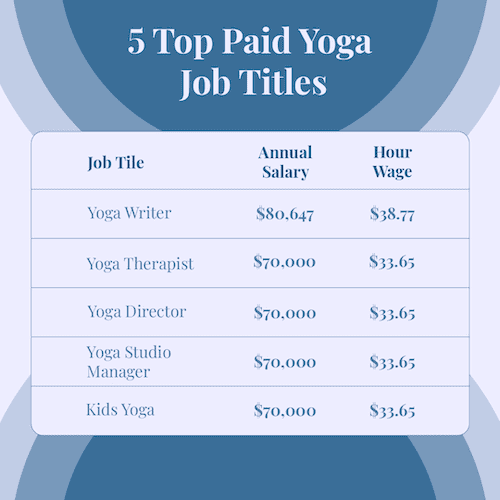
5 Top Paid Yoga Job Titles
Yoga instruction and yoga therapy can encompass a wide range of services, roles, and job duties. These can require varying responsibilities and qualifications, as well as earn different pay. A few of the top paid yoga-related job titles from ZipRecruiter are included below.
Private Yoga Therapy Practices vs. Yoga Therapy Clinics
Establishing a private yoga therapy practice can often mean charging higher rates for your services. In addition to considering your location, experience, and skill to help determine your rates, look at what other yoga therapists are charging as well as similar private practices. Knowing what acupuncturists, massage therapists, and psychotherapists charge in your city can help provide additional context for what a yoga therapist might charge.
Setting up a yoga therapy clinic, or even a couple of clinic days in your private practice, can be a way to serve different clientele with lower rates. If you’re operating as a yoga therapy clinic or setting aside clinic days, you could provide shorter appointments and charge less—perhaps 30-minute appointments rather than 60-minute appointments.
How Do Your Credentials and Yoga Therapy Certification Affect Salary?
You can’t just become a yoga expert overnight and begin collecting a yoga therapist salary with no issues. Additional years of industry experience will warrant higher wages. The ability to stand apart from the crowd in order to attract additional customers can convince your employer to provide a raise. Above all else, your industry credentials and overall training will determine your salary.
Achieving professional certification is usually the first step in bolstering your yoga salary. The International Association of Yoga Therapists (IAYT) provides important professional credentialing to those yoga therapists. These credentials will distinguish you as a true professional who has met the established standards of the IAYT.
Many first study yoga at the university level before embarking upon their professional careers, though this is not a necessary prerequisite with the right yoga therapy training. Even if you have a Bachelor’s of Arts in Yogic Studies or a Master of Science in Yoga Therapy, you’ll need to become certified by the IAYT to achieve much professional success. Your yoga therapy salary may depend on the level of professional certification you use to illustrate your skills to a prospective employer. Although there are costs to yoga therapy training and certification, they are important for increasing your earning potential.
An accredited institution approved by the IAYT can help you boost your yoga therapy salary.
Become a Certified Yoga Therapist With Breathing Deeply
Ready to begin your yoga therapy training and become a yoga therapist? Breathing Deeply Yoga Therapy offers accessible yoga therapy training, including an IAYT accredited advanced program. Our mission is to spread the availability of high-quality, practical, and ethical yoga therapy.
Apply today for one of our programs. A new Breathing Deeply class will be starting soon!











 As I reflect on our school and the changes we have gone through over the year, I am reminded of this quote from the father of modern yoga therapy. This year our student body has grown. Our Advanced Program has taken off and many of you are working on or submitting case studies. I have had the pleasure of working with you on how to effectively serve your yoga therapy clients. Through this, I have witnessed so many of you in a process of transformation.
As I reflect on our school and the changes we have gone through over the year, I am reminded of this quote from the father of modern yoga therapy. This year our student body has grown. Our Advanced Program has taken off and many of you are working on or submitting case studies. I have had the pleasure of working with you on how to effectively serve your yoga therapy clients. Through this, I have witnessed so many of you in a process of transformation.